chronic prostatitis- One of the most common diseases in adult men. Prostatitis significantly reduces quality of life and is the cause of psychosomatic and sexual disorders. The lack of adequate understanding of the nature of the disease makes the treatment of chronic prostatitis a daunting task that requires great patience from both the patient and his attending physician.
.jpg)
Classification
The National Institutes of Health (NIH USA) developed and proposed the followingClassificationChronic prostatitis:
- chronic bacterial prostatitis;
- Chronic nonbacterial prostatitis (with and without signs of inflammation);
- Chronic asymptomatic prostatitis.
Modern andrologists adhere to this classification in the diagnosis and treatment of inflammatory diseases of the prostate. Acute prostatitis stands out alone. Knowing which category the identified pathology falls into, physicians will be able to choose the best treatment options and achieve significant success in treating the disease.
Causes and Risk Factors
The distinction between bacterial and nonbacterial chronic prostatitis is not accidental. The various causes of disease determine the strategy of treatment and largely influence the outcome of the disease.
chronic bacterial prostatitis
Chronic bacterial prostatitis occurs in 10-15% of patients. The immediate cause of disease development is the entry of pathogenic and opportunistic flora into the prostate. By definition, the prostate is free of bacteria. Prostate infections may pass through the urethra as well as hematogenous and lymphatic infections. During inspections, the following microorganisms were most commonly detected:
- Escherichia coli (up to 95%);
- Proteus;
- Klebsiella;
- Pseudomonas.
Representatives of Gram-positive flora (Staphylococcus, Streptococcus) are very rare. In some cases, growth of two or more microorganisms is noted (co-infection). May be infected with pathogenic flora (Chlamydia, Trichomonas, Neisseria gonorrhoeae, etc. ).
Most of the microorganisms detected during the examination were representative of the normal microbial community. Under normal circumstances, they do not harm the body and exist peacefully on the mucous membranes of the urinary system and digestive tract. Under certain conditions, conditional pathogenic flora grow and multiply, causing inflammation of the prostate tissue and all symptoms of the disease.
risk factorThe development of chronic bacterial prostatitis:
- lack of personal hygiene;
- low temperature;
- genital trauma;
- Inflammatory diseases of the urinary system;
- The presence of sexually transmitted infections.
All of these result in a decrease in local and systemic immunity and in the natural proliferation of opportunistic flora in the prostate. In the case of inflammatory diseases of the reproductive tract, it is not excluded that the infection can enter through the urethra. The likelihood of developing prostatitis increases with existing urethritis, cystitis, and colitis.
chronic nonbacterial prostatitis
There are several theories about the occurrence of this disease:
- chemical inflammation theory. . . pouring urine into the prostate during urination can lead to urate deposits and the development of inflammation. Urethral strictures (stenosis) and other developmental abnormalities can promote urethral prostatic reflux.
- immunology. . . version based on autoimmune damage to prostate tissue due to exposure to bacterial antigens. The genetic predisposition to this pathological form was considered.
- neurogenic theory. . . violation of the innervation of the pelvic region can lead to stagnation of blood in the organs and lead to the development of prostatitis.
In the development of non-bacterial prostatitis, the following points also deserve special attention.risk factor:
- sedentary work;
- a sedentary lifestyle;
- bad habits;
- stress and emotional overload;
- Long-term abstinence.
These risk factors can cause prostate congestion, leading to impaired microcirculation in the pelvic organs. Microbial factors only play a role in the initial stages of disease development. In the future, its importance will decrease, and autoimmune processes and nutritional disorders in prostate tissue will come to the fore.
According to statistics, 85-90% of men suffer from non-bacterial chronic prostatitis (not directly related to infection with pathogenic or opportunistic bacteria).
symptom
Chronic prostatitis mainly occurs in men aged 25-40. The likelihood of developing this disorder increases with age. In old age, prostate inflammation is often combined with adenomas (benign tumors of the prostate).
SignChronic prostatitis:
- Dull pain in the lower abdomen;
- Irradiation for pain in the groin, scrotum, perineum, waist, sacrum;
- Increased discomfort during sex and bowel movements.
Urinary disturbances are very typical:
- frequent urination;
- Excretion of a small portion of urine;
- A feeling of incomplete emptying of the bladder;
- The appearance or intensification of pain during urination;
- Slow and intermittent urine flow.
The latter symptom is characteristic of prostate adenoma and usually occurs in the context of chronic prostatitis.
With the long-term development of the disease, there are obstacles in the sexual field:
- decreased libido;
- worsening erections;
- reduce the duration of sexual intercourse;
- premature ejaculation;
- abdominal pain after ejaculation;
- Lack of spontaneous morning erections.
Chronic prostatitis is one of the leading causes of erectile dysfunction, in which men are unable to achieve and maintain an erection sufficient for full intercourse. This condition can severely disrupt the course of life and can lead to depression and other psycho-emotional disorders.
Chronic asymptomatic prostatitis does not have any clinical manifestations. The disease was discovered incidentally during an examination by a urologist. Although asymptomatic, prostate inflammation can lead to serious complications, erectile dysfunction, and other health problems.
complication
Introduced prostatitis triggers the development of this condition:
- Prostate abscess;
- Cystitis and pyelonephritis (inflammation of the bladder and kidneys);
- vesiculitis (inflammation of the seminal vesicles);
- erectile dysfunction;
- Infertility.
The earlier a disease is detected and treatment begins, the greater the chance of a favorable outcome for the disease.
diagnosis
The following methods are used to detect chronic prostatitis:
Checked by a urologist
In individual appointments, doctors focus on the patient's complaint. Examine the external genitalia and perform a digital rectal examination of the prostate. On palpation, the doctor will assess the size and shape of the glands. In the case of chronic prostatitis, the organ enlarges slightly. This procedure is combined with the collection of prostate secretions for microbiological examination.
Four glass samples
The main method that allows you to identify the prostatic inflammatory process and differentiate it from other diseases. The collection of materials takes place in several stages. In the morning, after not going to the toilet for 5-6 hours, a man urinates in two jars - part one (initial) and part two (middle). In the first part, the contents of the urethra are washed away, and in the second part - the bladder. A third portion of urine is collected after a prostate massage and allows you to assess the condition of your prostate. The secrets of the prostate were collected separately for bacteriological culture.
In urinalysis, two parameters are evaluated: the number of white blood cells and red blood cells. With prostate disease, the white blood cell count in the third part of the urine is elevated. Usually, there are no more than 10 of them in the field of view.
Microbiological examination
When performing the three-cup test, not only the number of white blood cells is assessed, but the material is also taken for bacterial inoculation. The third part of urine is of particular interest to doctors if chronic prostatitis is suspected. Based on the test results, doctors can identify the causative agent of the disease and choose the best antibiotic treatment.
Detection of opportunistic bacteria with a titer greater than 10 has diagnostic value.3CFU/ml or detect any number of definite pathogenic microorganisms.
Prostate secretion bacterial culture
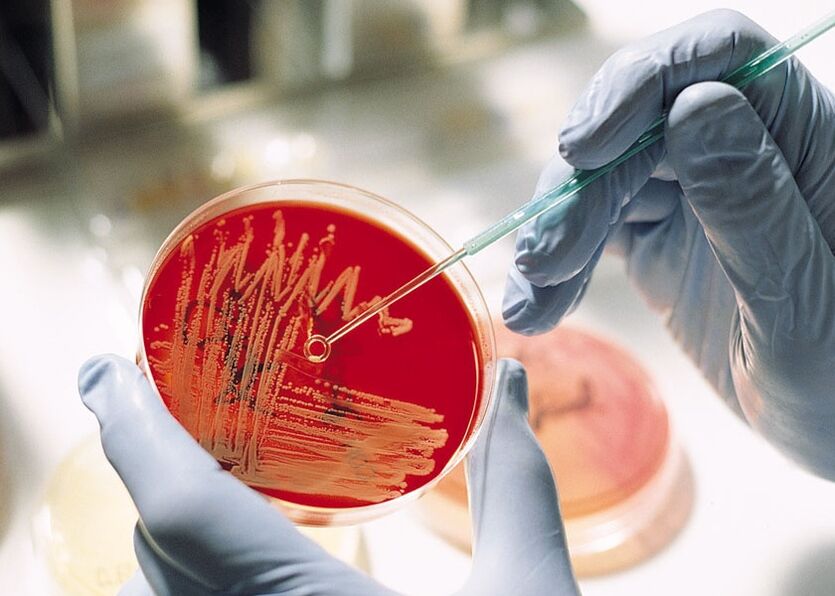
Before drawing a third portion of urine during prostate massage, the doctor will draw the secretions for bacteriological examination. The results obtained also allow you to determine diagnosis and treatment strategies.
Diagnostic criteria for chronic bacterial prostatitis:
- Identification of opportunistic microorganisms with titers greater than 10 in a third fraction of urine or prostate secretions3CFU/ml.
- The detection of opportunistic bacteria in the third part of urine or prostate secretions was significantly (10-fold) higher than in the second part of the urine.
- Part III Identification of pathogenic microorganisms in urine or prostate secretions.
Ultrasound
Ultrasonography allows you to assess the size of organs and identify accompanying pathology. Often, chronic prostatitis is combined with a prostate adenoma, a benign tumor.
Treatment principles
Treatment goals for chronic prostatitis are to eliminate inflammatory processes, activate blood flow and improve organ nutrition. When high titers of pathogenic or opportunistic microorganisms are detected, they are eliminated. Special attention is paid to lifestyle corrections and stimulation of body defenses.
medical treatement
For the treatment of chronic prostatitis, use the following methodsdrug:
- Antibiotics are selected taking into account the identified pathogens.
- Anti-inflammatory drugs reduce inflammation and reduce pain.
- Means to promote urination (alpha-blockers, which relax the muscles of the urethra and stimulate the flow of urine).
- Means of increasing blood flow to the pelvic organs.
The choice of antibiotic will depend on the identified pathogen. When selecting a drug, consideration should be given to its ability to penetrate the hematopoietic prostate barrier and accumulate in prostate tissue. These conditions are met by fluoroquinolones. Macrolides and tetracyclines are also used to treat chronic prostatitis.
According to the recommendations of the European Association of Urology, the course of antimicrobial therapy should be at least 2 weeks after the initial diagnosis.
Treatment lasts up to 4-6 weeks after the results of the bacteriological studies are received and the bacterial nature of the disease is confirmed. This method not only gets rid of the pathogens of the disease, but also prevents the recurrence of prostatitis.
Unfortunately, antibiotic treatment is not always effective. Many microorganisms successfully persist in the secretions of the prostate and acquire resistance to antibiotics. Bacteria form specialized biofilms and form microbial colonies covered with complex polysaccharide structures. Most antimicrobial drugs are unable to penetrate this biological barrier, greatly reducing the effectiveness of treatment. This problem can be avoided with the use of modern antibiotics, which not only penetrate and accumulate in prostate tissue, but also penetrate the biofilm to infect bacteria that are so heavily protected.
non-drug treatment
Among non-drug treatments, special attention is paid to prostate massage. The procedure stimulates the blood supply to the prostate, clears congestion and promotes the excretion of secretions. The combination of massage and long-term use of antibacterial drugs is the main method for relieving the uncomfortable symptoms of chronic prostatitis in men.
Influenced physical therapy methods are used in conjunction with pharmacodynamics to treat chronic prostatitis. Good results can be seen from the use of ultrasound, laser beams, radio waves and myoelectric stimulation. Prostate Shockwave Massage (UHM) is very popular. Physical therapy is especially suitable for erectile dysfunction as one of the complications of prostatitis.
The treatment of prostatitis should pay special attention to diet. The following foods should be excluded from the diet:
- alcohol;
- spicy, spicy food;
- Fried and fatty foods (including fatty meats and fish).
Salt intake is limited to 5 grams per day. Prioritize fresh vegetables and fruits, herbs. Steaming is recommended.
Dieting will speed recovery, strengthen your immune system, and help your body cope with the stress of antibiotics when treating an illness.
Ethnoscience
Not all men go to the doctor when symptoms of prostatitis appear. Often, men prefer a folk approach, drawing on a knowledge base from numerous forums and relying on the advice of friends, relatives, and neighbors. Neglecting one's own health, refusing appropriate antibiotic treatment and other traditional methods of exposure threatens the development of complications and general deterioration. Untreated prostatitis can lead to erectile dysfunction. Is it worth the risk if you can go to the doctor on time and solve the problem with minimal damage?
Of course, there are aspects of traditional medicine that deserve special attention. Modern urology recognizes the effectiveness of many herbal remedies in the treatment of chronic prostatitis. Experts recommend herbal preparations based on the following ingredients:
- pumpkin seed oil;
- round-leaf holly;
- garden parsley;
- St. John's wort perforation;
- goldenrod canada;
- licorice root;
- Echinacea.
These ingredients, alone or in combination, stimulate blood flow to the pelvic organs, clear congestion and stimulate the immune system.
Herbs do not remove pathogenic bacteria from the body, but they help eliminate the symptoms of the disease.
Combined with antibacterials and prostate massage, herbal remedies can significantly improve general condition and speed up recovery.
prevention
The following will help reduce your risk of chronic prostatitis:suggestion:
- Hypothermia of the whole body and genital area, pelvis and lower extremities are not allowed. Wearing thermal underwear is worthwhile during the colder months.
- It is necessary to observe intimate hygiene rules and use condoms to prevent sexually transmitted infections. The best infection prevention is to avoid casual sex.
- You should take care of your health and promptly treat any ailments in the genital area.
- Dieting (giving up spicy, fried and greasy foods) and keeping fit (exercise, fitness, walking) are not superfluous.
Regular checkups by a urologist (at least annually) are recommended for all men over the age of 30. If you experience any unpleasant symptoms, you should see your doctor as soon as possible.
FAQ
Can chronic prostatitis be cured?
Contrary to popular belief, chronic prostatitis can be successfully treated. If you follow all your doctor's advice, you can get rid of the unpleasant symptoms of prostatitis and significantly improve your quality of life.
Can chronic prostatitis be asymptomatic?
Yes, variants of this disease can only be detected after examination by a urologist.
Is partner's chronic prostatitis dangerous to women?
Sexually transmitted infections are often the cause of chronic prostatitis. If the pathogen is identified, both parties must receive treatment. Otherwise, there is a risk of infection and reduced effectiveness of treatment due to recurrence of the disease.
Can chronic prostatitis have sex?
Yes, if the general situation allows and there are no problems in the sexual area (erectile dysfunction).
Can a child with chronic prostatitis be pregnant?
Yes, if the function of the prostate is preserved and its secrets are fully exploited. Before pregnancy, examination and treatment by a urologist is recommended. Infections that lead to the development of prostatitis are easily contagious to women. Intrauterine infection of the fetus can lead to abnormal development and termination of pregnancy.
How does chronic prostatitis affect potency?
Chronic inflammation of the prostate threatens the development of erectile dysfunction. In this pathological condition, libido decreases, erection frequency and intensity decrease, and orgasm becomes painful. In advanced cases, sexual activity becomes impossible.
Can chronic prostatitis be cured without antibiotics?
Antibiotic therapy is considered one of the key treatments for chronic prostatitis. In most cases, it is impossible to deal with the disease without antibiotics.
Can chronic prostatitis be cured with folk remedies?
It is impossible to get rid of chronic prostatitis with traditional medicine alone. For best results, complex treatments are performed using antibiotics, herbal preparations, anti-inflammatory drugs, and physical therapy.






























